CNS Stimulants: Few Interactions, Significant Repercussions
As with any pharmacologic class, central nervous system stimulants carry the risk of potential drug interactions that can be pharmacokinetic or pharmacodynamic.
INTRODUCTION
As with any pharmacologic class, central nervous system (CNS) stimulants carry the risk of potential drug interactions that can be pharmacokinetic (PK) or pharmacodynamic (PD).
Psychostimulants, like amphetamines and methylphenidate, are FDA approved to treat attention- deficit/hyperactivity disorder (ADHD).1,2In addition, modafinil and armodafinil are indicated to treat excessive somnolence due to narcolepsy, shift work disorder, and obstructive sleep apnea.3,4
About 3% of children aged 3 to 18 years receive pharmacological treatment for ADHD,5and these drugs are often used in combination with other medications.6Most stimulants are metabolized by CYP450 enzymes, and many can induce or inhibit these enzymes. Together, the prevalence of use and PK factors contribute to drug interaction potential.
PHARMACOKINETICS
Amphetamines and methylphenidate work by inhibiting dopamine and norepinephrine reuptake, and both impede monoamine oxidase (MAO).7This interaction is a potential source of many PD interactions with drugs that alter neurotransmitter levels or MAO activity.
Amphetamines are metabolized extensively by the CYP450 system, the majority of which is through CYP2D6.8About 7% of Caucasians are slow 2D6 metabolizers; and the prevalence is higher in Latinos and African Americans.7Given the large number of drugs that modify CYP2D6 activity and genetic polymorphisms that affect metabolizer status, amphetamine use has the potential for PK interactions. Methylphenidate is metabolized by hepatic and peripheral esterases, therefore CYP interactions are less likely.7
Modafinil and armodafinil have extensive involvement in the CYP P450 system. Both are metabolized, to some extent, by CYP3A4 and inhibit CYP2C9 and 2C19. Modafinil, however, induces CYP3A4 and CYP1A2, while armodafinil only induces 3A4.9,10
DRUG INTERACTIONS
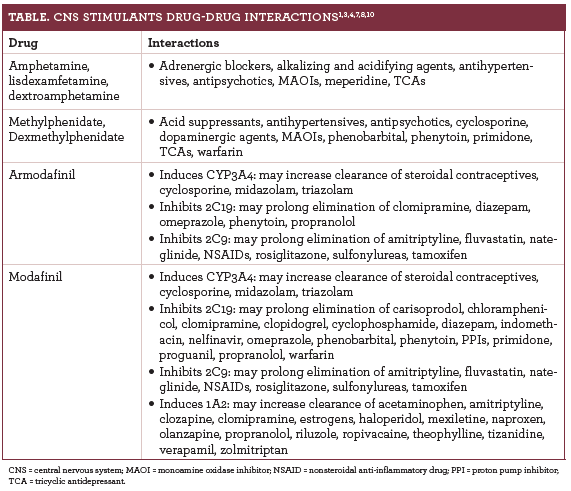
Table1,3,4,7,8,10summarizes important drug—drug interactions involving CNS stimulants. MAO inhibitors are contraindicated with amphetamines and methylphenidate. Concurrent use of these medications risks serious consequences, including hypertensive crisis and death. Prescribers should allow a significant drug washout period between these agents if they must be used simultaneously.8
Clinicians should cautiously prescribe drugs that alter the pH of the urine in patients taking amphetamines, as the elimination of the urine can be significantly altered. Acidifying drugs increase elimination, while alkalinizing drugs decrease it. In addition, amphetamine absorption increases with gastric alkalinizing agents like sodium bicarbonate and antacids. Co-administration of these medications should be avoided, and patients should be monitored for changes in the clinical effects related to their use.2,8
Psychostimulants can increase heart rate and blood pressure and may antagonize the effects of antihypertensives. Therefore, practitioners should closely monitor blood pressure in patients taking these medications.1,2,7
Methylphenidate’s prescribing information warns of the potential for PD interactions with dopaminergic agents like levodopa, tricyclic antidepressants, and antipsychotics.1The central stimulatory effects of amphetamines can be blocked with co-administration of antipsychotics, like haloperidol and chlorpromazine.2
Clinicians should carefully monitor patients with seizure disorders if they are receiving concomitant psychostimulants. Methylphenidate inhibits phenytoin metabolism and amphetamines may delay intestinal absorption of phenytoin and phenobarbital.1,2
Close therapeutic drug monitoring of warfarin and cyclosporine levels also is warranted for patients taking methylphenidate. The does of both medications may need to be reduced.10
Further, it is important to note any drugs in a patient’s medication list that induce or inhibit CYP3A4, as these can decrease or increase, respectively, the effects of modafinil and armodafinil.10Hormonal contraceptives are metabolized by 3A4, so patients are advised to use an alternative or concomitant method of birth control when using modafinil or armodafinil and for 1 month after, as their effects can persist even after discontinuation. Close monitoring of cyclosporine levels is also recommended.3,4
PRESCRIBING CONSIDERATIONS
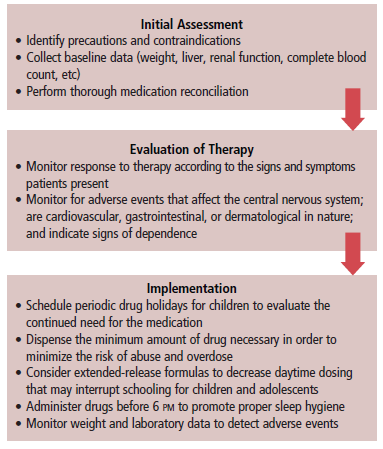
The flowchart presents considerations when prescribing CNS stimulants.5,11
ABUSE POTENTIAL
Amphetamines and methylphenidate both have abuse potential. They are ranked eighth and 13th, respectively, for substances known to cause dependence. About 25% of adolescents and adults have either diverted or abused these dugs.7According to the National Institute on Drug Abuse, 6.7% of high school seniors have used amphetamines and 1.2% have used methylphenidate without a prescription.12
Health care professionals have a responsibility to educate patients about this risk of abuse and dependence and to recognize its signs. The Medicine Abuse Project (medicineabuseproject.org) provides myriad resources about prescription drug abuse for families, educators, communities, law enforcement, and health care providers, including information about abuse, educational materials for patients, clinical guidelines, and screening tools.13
Leah Mangini, PharmD, is a PGY1 pharmacy practice resident at Baystate Medical Center, Springfield, Massachusetts.

