OTC and Homeopathic Options for Acute Cough
On any given day, it is typical to see parents waiting at doctor’s offices, urgent care facilities, and retail health locations with children who are experiencing a cough, as it is one of the most common symptoms for which patients seek primary care.
On any given day, it is typical to see parents waiting at doctor’s offices, urgent care facilities, and retail health locations with children who are experiencing a cough, as it is one of the most common symptoms for which patients seek primary care.1Cough can disrupt the lives of patients and entire families. A cough can keep a patient up all night, causing fatigue and disturbing work and school activities.
In 2014, more than $7 billion were spent in the United States on OTC medications to treat upper respiratory tract infection (URTI), including cough symptoms.2In addition, patients with URTI and cough symptoms come to retail clinics looking for something to relieve their symptoms.
Upper Respiratory Tract Infection
URTI, also known as the common cold, is one of the most common illnesses behind acute cough, or a cough that lasts less than 3 weeks. More than 200 different viruses can cause URTI. Among all of these viruses, however, rhinoviruses cause the majority of colds. Generally, children develop 6 to 8 URTIs per year, whereas adults develop 2 to 4 URTIs per year.
URTIs are most prevalent from September through March, although infection is possible at any time of year. Symptoms usually begin with sore throat and rhinorrhea followed by coughing, sneezing, watery eyes, headache, and body aches. Because URTIs are self-limiting, most infected individuals recover within 7 to 10 days. In those with weakened immune systems, asthma, or other respiratory conditions, however, serious illness such as pneumonia may develop.
The first line of management for patients with acute cough is to consider possible life-threatening conditions, such as pneumonia, severe exacerbation of asthma, chronic obstructive pulmonary disease, pulmonary embolism, and congestive heart failure. Despite the fact that 90% of acute cough cases are caused by viral infections,3the provider must conduct a thorough evaluation focusing on vital signs. A patient who is afebrile and does not have tachycardia or tachypnea is less likely to have pneumonia.
It is also important to conduct a thorough pulmonary exam to assess lung sounds. In acute bronchitis, wheezing may be present. If rales, egophony, or fremitus are detected, however, pneumonia needs to be considered and further evaluation must be completed (Table 13).
Table 1: Possible Signs of Pneumonia3
Fever (>38° C)
Tachypnea(>24 breaths/min)
Tachycardia(>100 bpm)
Evidence of consolidation on chest exam, such as rales, egophony, and fremitus
Cough is a very important function because it clears the airway of obstructive material. It is a reflex response to mechanical, chemical, or inflammatory irritation in the airway.4Cough receptors line the larynx and the tracheal bifurcations but decrease in number farther down the respiratory tract. This cough reflex works mainly in the larger airway. Material or fluid from the lower airways can move to the level of the larger airways, however, where coughing can be beneficial for removing material from the respiratory tract.5
Different pathways may be used to initiate the cough reflex. These include the afferent pathway, the central pathway (also known as the cough center), and the efferent pathway.5The specific pattern of cough depends on the site and type of stimulation. This is an important factor because medications may affect the pathways differently, yielding varied antitussive responses.
OTC Medications
A number of OTC medications are available in multiple formulations to relieve cough symptoms in children and adults (Table 2).
Table 2: OTC Medication for Cough Symptoms
Medication
Dosing
Adults
Children
Dextromethorphan (Delsym 12 Hour Cough Relief)
10 mL every 12 hours, not to exceed 20 mL in 24 hours
Age ≥12 years:
10 mL every 12 hours, not to exceed 20 mL in 24 hours
Age 6—11 years:
5 mL every 12 hours, not to exceed 10 mL in 24 hours
Age 4­—6 years:
2.5 mL every 12 hours, not to exceed 5 mL in 24 hours
Age <4 years: not recommended
Naproxen sodium
One 220-mg capsule every 12 hours as needed
Age ≥12 years:1 capsule every 12 hours as needed
Age ≤11 years:not recommended
Dimetapp Cold and Cough
Active ingredients (per 10 mL):
- Brompheniramine maleate, 2 mg (antihistamine)
- Dextromethorphan HBr, 10 mg (cough suppressant)
- Phenylephrine HCl, 5 mg (nasal decongestant)
20 mL every 4 hours
Age ≥12 years:
20 mL every 4 hours
Age 6—11 years:
10 mL every 4 hours
Age <6 years:
not recommended
Nasal saline
If the bottle tip touches the nose, clean it under hot water and dry off prior to recapping
1—2 sprays in each nostril as needed
Children:
1­—2 sprays each nostril as needed to relieve congestion
Infants:
Use drop application: 1-2 drops each nostril with gentle bulb syringe suction to extract mucus
First-Generation Antihistamine/Decongestant Combination
Postnasal drip in URTI may be a contributing factor to cough because it may increase the sensitivity of the afferent sensory nerves in the upper airway. First-generation antihistamine and decongestant combination use in URTI has led to quicker improvement of postnasal drip, throat clearing, and coughing. In contrast, study results have shown no efficacy for newer generation antihistamines in reducing cough and cold symptoms.6Some of the side effects of first-generation antihistamines include dry mouth, drowsiness, dizziness, urinary retention, and headache.
Codeine
Codeine suppresses the cough reflex through a direct effect on the cough center.7While codeine has been widely recognized as the gold standard for cough suppression, recent research has produced different findings. For instance, results of several double-blind, placebo-controlled studies failed to show a significant cough-suppressing effect with codeine compared with placebo.8In one randomized, controlled trial with 82 adult patients with acute cough from URTI, results showed no significant difference between codeine and placebo in treating cough. This particular study examined 3 separate means of measuring cough to judge improvement: cough—sound–pressure levels, cough frequency, and a subjective symptom score.9
The FDA is investigating the use of codeine-containing medication to treat cough in children and teens younger than 18 years because of the potential for serious side effects. In April 2015, the European Medicines Agency stated that codeine must not be used to treat cough and cold in children younger than 12 years, and the agency discouraged its use in children aged 12 to 18 years with a history of asthma or other breathing problems.10
Dextromethorphan
Dextromethorphan works like codeine in the cough center, but it does not have the addictive potential of codeine. In adults, dextromethorphan cough suppression potency is nearly equal to that of codeine.4Dextromethorphan can be purchased OTC in multiple products. It is not recommended for children younger than 4 years.
Naproxen
In a randomized, double blind, placebo-controlled trial of an experimentally induced rhinovirus common cold, the nonsteroidal anti-inflammatory drug naproxen decreased cough as well as headache, malaise, and myalgia.11
Homeopathic Remedies
Besides OTC medication, many home remedies can help relieve cough and cold symptoms (Table 3).
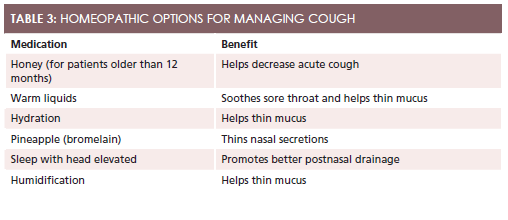
Although honey is safe for children aged 1 year and older, its efficacy in relieving cough is questionable. A pair of randomized, controlled trials involving 265 children compared honey with dextromethorphan, diphenhydramine, and no treatment, and the results showed that honey was better than no treatment, slightly better than diphenhydramine, and equal to dextromethorphan in reducing frequency of cough.12While honey is worth recommending to patients and parents of children with acute cough, parents and caretakers should be reminded not to give honey to children younger than age 1 due the risk forClostridium botulinuminfection.
Patients with acute cough should be encouraged to stay hydrated because it can help thin mucus. The best options for hydration are water, juice, and broth, though another option is warm lemon water with honey. It is a myth that drinking milk will thicken or produce more phlegm, so it is okay to continue giving children milk to prevent dehydration in URTI. Alcohol, coffee, and soda, which can increase dehydration, should be avoided.
Pineapple contains an enzyme called bromelain, which appears to thin nasal secretions and has been shown to be an effective mucolytic agent. Results of a German clinical study found that children with acute sinusitis showed statistically significant faster symptom recovery with pineapple.13In addition to pineapple, saline can help thin nasal secretions.
Older children and adults should also be encouraged to sleep with an extra pillow to help with increased postnasal drainage. This may help decrease some of the cough at night. In addition, humidification will help loosen nasal congestion. Adding moisture via a humidifier in the home is helpful, especially during the drier winter months. Patients should be instructed to change the water daily and follow manufacturer recommendations for changing filters.
Conclusion
There is no good time to be sick. Providers often hear, “I have a huge work meeting in a few days” or “I go on vacation in 3 days, so I have to get better now.” Patient education is very important along with antibiotic stewardship. Acute cough is almost always viral and does not require antibiotics. Patients should be educated about OTC medications along with homeopathic options. These remedies will help relieve cough and cold symptoms while the body fights the viral infection.
Melissa Bushgraduated from the University Missouri-Kansas City with her master’s degree in nursing education in 2004 and her family nurse practitioner certification in 2005. She has worked for 10 years at Minute Clinic helping her patients on their path to better health.
References
- De Blasio F, Virchow JC, Polverino M, et al. Cough management: a practical approach.Cough. 2011;7(1):7. www.coughjournal.com/content/7/1/7. Accessed March 6, 2016.
- OTC sales by category 2011-2014. Consumer Healthcare Products Association website. www.chpa.org/OTCsCategory.aspx. Accessed March 6, 2016.
- Acute cough illness (acute bronchitis). CDC website. cdc.gov/getsmart/community/materials-references/print-materials/hcp/adult-acute-cough-illness.pdf. Accessed March 6, 2016.
- American Academy of Pediatrics Committee on Drugs. Use of codeine- and dextromethorphan-containing cough remedies in children.Pediatrics.1997;99(6):918-920. http://pediatrics.aappublications.org/content/99/6/918. Accessed March 6, 2016.
- Polverino M, Polverino F, Fasolino M, Andò F, Alfieri A, De Blasio F. Anatomy and neuro-pathophysiology of the cough reflex arc.Multidiscip Respir Med. 2012;7(1):5. doi: 10.1186/2049-6958-7-5. ncbi.nlm.nih.gov/pmc/articles/PMC3415124/. Accessed March 6, 2016.
- Pratter M. Cough and the common cold: ACCP evidence-based clinical practice guidelines.Chest.2006;129(suppl 1):72S-74S.
- Pharmacovigilance Risk Assessment Committee. Codeine containing medicinal products for the treatment of cough and/or cold in paediatric patients. European Medicines Agency website. www.ema.europa.eu/docs/en_GB/document_library/Referrals_document/Codeine_cough_or_cold_in_children/Recommendation_provided_by_Pharmacovigilance_Risk_Assessment_Committee/WC500186522.pdf. Published March 12, 2015. Accessed March 6, 2016.
- Bolser DC, Davenport PW. Codeine and cough: an ineffective gold standard.Curr Opin Allergy Clin Immunol. 2007;7(1):32-36.
- Goldman RD. Codeine for acute cough in children.Can Fam Physician. 2010;56(12):1293-1294.
- FDA Drug Safety Communication: FDA evaluating the potential risks of using codeine cough-and-cold medicines in children. FDA website. www.fda.gov/Drugs/DrugSafety/ucm453125.htm. Updated January 16, 2016. Accessed March 6, 2016.
- Sperber SJ, Hendley JO, Hayden FG, Riker DK, Sorrentino JV, Gwaltney JM Jr. Effects of naproxen on experimental rhinovirus colds. A randomized, double-blind, controlled trial.Ann Intern Med. 1992 Jul 1;117(1):37-41.
- Goldman RD. Honey for treatment of cough in children.Can Fam Physician. 2014;60(12):1107-1108,1110.
- Helms S, Miller A. Natural treatment of chronic rhinosinusitis.Alt Med Rev. 2006;11(3):196-207.

