They Are What They Eat: Children and Drugs
Health care providers should be aware of drug–food interactions that affect medication effectiveness.
About 27% of american children live with chronic diseases.1As the number of illnesses continues to rise, health care professionals must ensure that pediatric patients receive optimal medication therapy. Health care providers should be aware of drug—food interactions that affect medication effectiveness. Foods contain active substances that interact with certain medications, producing unexpected adverse effects. An interaction’s impact depends on medication-related factors, such as dose and timing, and patient-related factors, such as age, health, and size. Consequences also vary from one case to another. Drug–food interactions can delay, decrease, or enhance drug absorption. Patients can experience adverse effects or toxicity or may not receive the medication’s full therapeutic benefit.2
Drug—food interactions occur using 4 different mechanisms (see Table 1).2,3
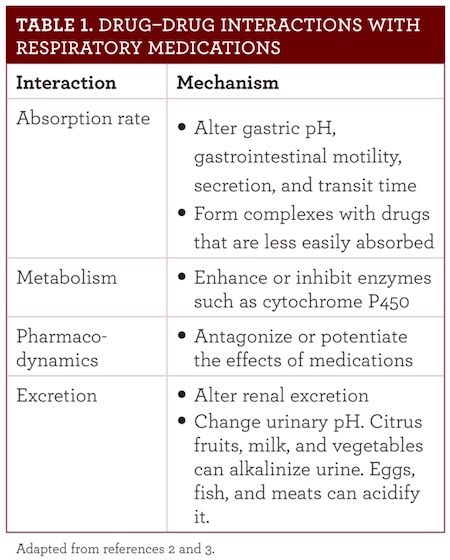
Unfortunately, diseases among children are common, and the list of medications used is long. Five dietary components have many drug interactions in children. These are:
Caffeine.Attention-deficit/hyperactivity disorder (ADHD) affects 1 in 10 children, so amphetamine use is common.1Caffeine interacts with amphetamines because it is a xanthine and hence a central nervous system stimulant.1Caffeine also interacts with albuterol and pseudoephedrine by releasing catecholamines such as adrenaline, synergizing their effects, and causing an increase in blood pressure (BP). Being a cytochrome P450 1A2 metabolite, caffeine also interacts with drugs such as ciprofloxacin. Caffeine is an ingredient in many foods and drinks. Reading product labels and limiting the use of caffeine while taking these medications is recommended.2
Dairy.Children often receive antibiotics for acute events such as ear and throat infections. Their use is more common than ever because cancer is the leading cause of death by disease in children.1Cancer and its treatment can cause neutropenia and thrombocytopenia, leading to infections requiring antibiotics.
Dairy products have a high content of metallic ions such as aluminum, bismuth, calcium, and iron.3These ions, especially calcium, decrease the absorption of certain antibiotics by causing chelation. Popular foods among kids, such as cheese, ice cream, milk, and yogurt, bind to the antibiotics, forming complexes that prevent them from entering the circulation. Dairy products reduce doxycycline, minocycline, and tetracycline levels by 80%. Dairy also chelates quinolones, such as ciprofloxacin, up to 40%. Separating the antibiotic dose from dairy products by 2 to 3 hours avoids this interaction.
Grapefruit juice.Among citrus fruit drinks, grapefruit juice interacts with antihistamines, BP drugs, thyroid replacement drugs, stomach acid—blocking drugs, and cough suppressants such as dextromethorphan. Grapefruit juice contains furanocoumarins, which alter the characteristics of these medications.4With chronic diseases and disorders such as ADHD, diabetes, heart disease, and obesity on the rise, spacing grapefruit juice intake with medications by at least 4 fours is very important in the pediatric population.
Potassium-rich foods.With the increase in juvenile diabetes, pediatric patients are experiencing an increase in both hypertension and renal dysfunction.1About 90% of Americans 2 years and older consume too much sodium, which increases the risk of hypertension.5To avoid this risk, use of salt substitutes such as LoSalt, which replace the sodium with potassium, has increased. Potassium-rich foods, including bananas, green leafy vegetables, oranges, and salt supplements, have the potential to cause drug interactions with angiotensin-converting enzyme inhibitors and potassium-sparing diuretics.4These drugs increase potassium. Combining them with dietary potassium can lead to hyperkalemia, causing irregular heartbeats and palpitations. Children on these classes of antihypertensives should limit their consumption of foods high in potassium.
Soybean products.Soybean products, such as milk, tofu, sauces, and even baby formula, have become a staple in many American households. These products have the potential to cause drug—food interactions. For example, hormone replacement therapy is employed in children for diseases that may cause hormone deficiencies, such as cancer and diabetes. Soy products decrease the absorption of estrogens, levothyroxine, and progestins.3Separating doses by at least 4 hours can avoid this drug—food interaction.
Many soy products have a high tyramine content. Monoamine oxidase inhibitors are rarely used in the pediatric population, and when they are, patients must avoid concurrent use of soy products. Too much tyramine can lead to a life-threatening hypertensive crisis.2
Heart disease is the fifth-leading cause of death in 1- to 5-year- olds.1Soybeans are rich in vitamin K, which can decrease warfarin’s effectiveness. Children who are on warfarin should limit soy products and need regular blood monitoring.3
HEALTH CARE PROVIDERS’ ROLE
Medication use in children continues to increase because of the rise in chronic diseases and disorders such as cancer, diabetes, high BP, neurodevelopmental disorders, and obesity. The Joint Commission expects health care providers to identify potential drug—food interactions, avoid harm to patients, and note potential interactions in the medical record.2Table 2 summarizes common food—drug interactions.2-4
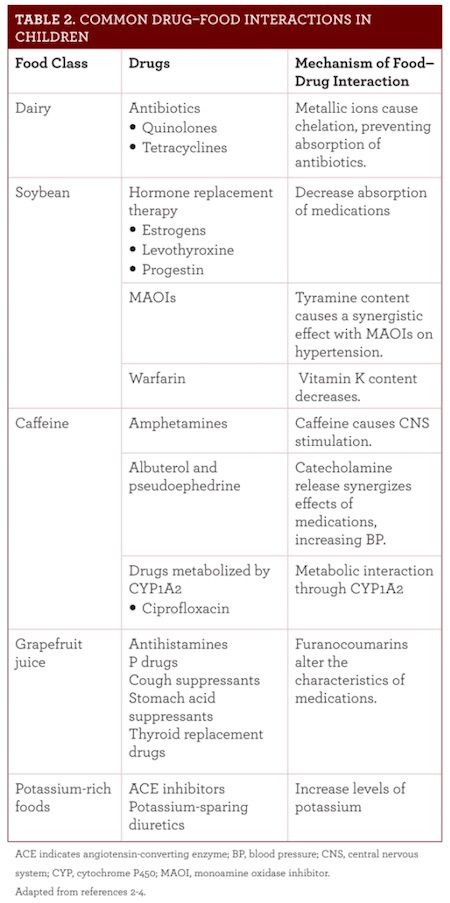
All health care professionals, such as nurses, pharmacists, and physicians, should work together to prevent drug—food interactions. Inquiring about the patient’s diet and being mindful of it when prescribing medications can prevent drug–food interactions. Counseling the patient and providing resources, such as medication guides, can optimize their therapy.
Blerina Mukallari is a PharmD candidate at the University of Connecticut School of Pharmacy in Storrs.

